Clinical application of expanded internal mammary artery perforator flap combined with vascular supercharge in reconstruction of faciocervical scar
-
摘要:
目的 总结扩张的胸廓内动脉穿支(IMAP)皮瓣联合血管增压在面颈部瘢痕整复中的临床应用经验。 方法 采用回顾性观察性研究方法。2012年9月—2021年5月,上海交通大学医学院附属第九人民医院收治23例符合入选标准的烧创伤后面颈部瘢痕患者,其中男18例、女5例,年龄11~58岁,均采用扩张的IMAP皮瓣整复。Ⅰ期根据瘢痕部位和范围在前胸置入1个或2个合适额定容量的皮肤软组织扩张器,术中注意保护IMAP、锁骨上动脉胸支和胸外侧动脉,术后注入生理盐水进行扩张。Ⅱ期行皮瓣转移术,术前使用彩色多普勒超声血流探测仪明确优势IMAP。切除面颈部瘢痕,形成面积为9 cm×7 cm~28 cm×12 cm的创面,术中注意保留颞浅动静脉或面动静脉穿支。以优势IMAP为蒂,根据瘢痕切除后创面面积和位置设计皮瓣:对于中小面积的创面,采用IMAP单蒂皮瓣转移修复;对于缺损面积较大者,利用吲哚菁绿血管造影(ICGA)评价前胸各血管的供血范围,当IMAP不足以供养整块皮瓣时,利用锁骨上动脉胸支或胸外侧动脉进行血管增压,设计双蒂皮瓣。根据供受区间的距离,选择带蒂或游离转移皮瓣。转移皮瓣后再次行ICGA判断皮瓣血供。将供瓣区直接拉拢缝合。统计皮肤软组织扩张器置入个数、额定容量、注射生理盐水量和扩张周期,优势IMAP位置,采用皮瓣总个数和不同血管蒂类型皮瓣个数、皮瓣面积,Ⅱ期术后皮瓣存活情况、供受区常见并发症发生情况和随访情况。 结果 共置入25个皮肤软组织扩张器,皮肤软组织扩张器额定容量为200~500 mL,注射生理盐水量855~2 055 mL,扩张周期4~16个月。术前在第2肋间(20侧)或第3肋间(5侧)探及优势IMAP。共切取25个扩张皮瓣,其中2个IMAP带蒂皮瓣、11个IMAP游离皮瓣、4个锁骨上动脉胸支带蒂+IMAP游离皮瓣、8个IMAP+胸外侧动脉游离皮瓣,皮瓣面积10 cm×8 cm~30 cm×14 cm。Ⅱ期术后3例患者出现皮瓣尖端坏死,经常规换药后愈合;1例患者IMAP和面动脉吻合处出现血管蒂局部扭转、血栓栓塞,手术探查取出血栓、重新吻合血管后,血供恢复正常。14例患者在Ⅱ期术后1~6个月进行了皮瓣修薄手术。随访4个月~9年,所有患者皮瓣外观良好,面颈部功能改善,供区可见线性瘢痕形成;1例女性患者出现明显乳头移位,双侧乳房不对称。 结论 扩张IMAP皮瓣颜色、质地与面颈部皮肤组织匹配,且切取后对胸部供区的损伤小,联合血管增压可灵活设计双蒂皮瓣,进一步改善血供,扩大皮瓣切取面积,是大面积面颈部瘢痕整复的良好选择。 Abstract:Objective To summarize the clinical experience of expanded internal mammary artery perforator (IMAP) flap combined with vascular supercharge in reconstruction of faciocervical scar. Methods The retrospective observational study was conducted. From September 2012 to May 2021, 23 patients with postburn or posttraumatic faciocervical scars who met the inclusion criteria were admitted to Shanghai Ninth People's Hospital of Shanghai Jiao Tong University School of Medicine, including 18 males and 5 females, aged from 11 to 58 years, all of whom were reconstructed with expanded IMAP flaps. At the first stage, one or two skin and soft tissue expander (s) with appropriate rated capacity were implanted in the anterior chest area according to the location and size of the scars. The IMAP, thoracic branch of supraclavicular artery, and lateral thoracic artery were preserved during the operation. The skin and soft tissue expanders were inflated with normal saline after the operation. The flaps were transferred during the second stage. The dominant IMAP was determined preoperatively using color Doppler ultrasound (CDU) blood flow detector. The faciocervical scars were removed, forming wounds with areas of 9 cm×7 cm-28 cm×12 cm, and the perforators of superficial temporal artery and vein or facial artery and vein were preserved during the operation. The flaps were designed according to the area and size of the wounds after scar resection with the dominant IMAP as the pedicle. Single-pedicle IMAP flaps were used to repair small and medium-sized wounds. For larger defects, the blood perfusion areas of vessels in the anterior chest were evaluated by indocyanine green angiography (ICGA). In situations where the IMAP was insufficient to nourish the entire flap, double-pedicle flaps were designed by using the thoracic branch of supraclavicular artery or lateral thoracic artery for supercharging. Pedicled or free flap transfer was selected according to the distance between the donor areas and recipient areas. After transplantation of flaps, ICGA was conducted again to evaluate blood perfusion of the flaps. The donor sites of flaps were all closed by suturing directly. Statistics were recorded, including the number, rated capacity, normal saline injection volume, and expansion period of skin and soft tissue expanders, the location of the dominant IMAP, the total number of the flaps used, the number of flaps with different types of vascular pedicles, the flap area, the flap survival after the second stage surgery, the occurrence of common complications in the donor and recipient areas, and the condition of follow-up. Results Totally 25 skin and soft tissue expanders were used in this group of patients, with rated capacity of 200-500 mL, normal saline injection volume of 855-2 055 mL, and expansion period of 4-16 months. The dominant IMAP was detected in the second intercostal space (20 sides) or the third intercostal space (5 sides) before surgery. A total of 25 expanded flaps were excised, including 2 pedicled IMAP flaps, 11 free IMAP flaps, 4 pedicled thoracic branch of supraclavicular artery+free IMAP flaps, and 8 free IMAP+lateral thoracic artery flaps, with flap areas of 10 cm×8 cm-30 cm×14 cm. After the second stage surgery, tip necrosis of flaps in three patients occurred, which healed after routine dressing changes; one patient developed arterial embolism and local torsion on the vascular pedicle at the anastomosis of IMAP and facial artery, and the blood supply recovered after thrombectomy and vascular re-anastomosis. Fourteen patients underwent flap thinning surgery in 1 month to 6 months after the second stage surgery. The follow-up for 4 months to 9 years showed that all patients had improved appearances of flaps and functions of face and neck and linear scar in the donor sites of flaps, and one female patient had obvious nipple displacement and bilateral breast asymmetry. Conclusions The expanded IMAP flap is matched in color and texture with that of the face and neck, and its incision causes little damage to the chest donor sites. When combined with vascular supercharge, a double-pedicle flap can be designed flexibly to further enhance the blood supply and expand the flap incision area, which is a good choice for reconstruction of large faciocervical scar. -
Key words:
- Surgical flaps /
- Face /
- Neck /
- Cicatrix /
- Perforator flap /
- Internal mammary artery /
- Skin and soft tissue expansion /
- Vascular supercharge
-
参考文献
(34) [1] AkitaS,HayashidaK,TakakiS,et al.The neck burn scar contracture: a concept of effective treatment[J/OL].Burns Trauma,2017,5:22[2022-03-16]. https://pubmed.ncbi.nlm.nih.gov/28717655/. DOI: 10.1186/s41038-017-0086-8. [2] GreenhalghDG.Management of facial burns[J/OL].Burns Trauma,2020,8:tkaa023[2022-03-16].https://pubmed.ncbi.nlm.nih.gov/32665953/. DOI: 10.1093/burnst/tkaa023. [3] HoWS,YingSY.An epidemiological study of 1063 hospitalized burn patients in a tertiary burns centre in Hong Kong[J].Burns,2001,27(2):119-123.DOI: 10.1016/s0305-4179(00)00095-4. [4] LiQ,ZanT,GuB,et al.Face resurfacing using a cervicothoracic skin flap prefabricated by lateral thigh fascial flap and tissue expander[J].Microsurgery,2009,29(7):515-523.DOI: 10.1002/micr.20640. [5] BakamjianVY. A two-stage method for pharyngoesophageal reconstruction with a primary pectoral skin flap[J].Plast Reconstr Surg, 1965,36:173-184. DOI: 10.1097/00006534-196508000-00004. [6] 卢燕雪,罗盛康.胸廓内动脉及其穿支的解剖与临床应用研究进展[J].中国临床解剖学杂志,2019,37(5):597-599.DOI: 10.13418/j.issn.1001-165x.2019.05.025. [7] AngrigianiC,RancatiA,VarelaI,et al.The deltopectoral/internal mammary artery perforator flap revisited: design variations based on cadaveric and clinical investigation[J].Ann Plast Surg,2022,88(1):88-92.DOI: 10.1097/SAP.0000000000002863. [8] MaX,LiY,LiW,et al.Reconstruction of facial-cervical scars with pedicled expanded deltopectoral flap[J].J Craniofac Surg,2017,28(6):1554-1558.DOI: 10.1097/SCS.0000000000003901. [9] WongS,GogginJD,WebsterND,et al.Pre-expanded internal mammary artery perforator flap[J].Clin Plast Surg,2017,44(1):65-72.DOI: 10.1016/j.cps.2016.09.001. [10] ZanT,LiH,GuB,et al.Surgical treatment of facial soft-tissue deformities in postburn patients: a proposed classification based on a retrospective study[J].Plast Reconstr Surg,2013,132(6):1001e-1014e.DOI: 10.1097/PRS.0b013e3182a97e81. [11] 王占统,董琛,唐银科,等.预扩张胸三角皮瓣修复面颈部病损的临床效果[J].中华烧伤杂志,2020,36(5):363-369.DOI: 10.3760/cma.j.cn501120-20200113-00019. [12] 鲁开化,马显杰,艾玉峰,等. 扩张后的胸三角皮瓣修复面颈部瘢痕[J]. 中华整形烧伤外科杂志,1996,12(3):187-189. [13] 马显杰, 丁健科. 皮肤软组织扩张术在儿童体表病损修复中的应用[J]. 中华烧伤与创面修复杂志,2022, 38(4): 301-305. DOI: 10.3760/cma.j.cn501120-20211019-00359. [14] KhoongYM,HuangX,GuS,et al.Imaging for thinned perforator flap harvest: current status and future perspectives[J/OL].Burns Trauma,2021,9:tkab042[2022-03-16].https://pubmed.ncbi.nlm.nih.gov/34926708/.DOI: 10.1093/burnst/tkab042. [15] WangZ,DingJ,TangY,et al.Application of various methods to evaluate the postoperative characteristics of expanded pedicled deltopectoral flap for large facial scars[J/OL].J Craniofac Surg,2021(2021-09-22)[2021-09-28].https://pubmed.ncbi.nlm.nih.gov/34560753/.DOI:10.1097/SCS.0000000000008221.[pub- lished online ahead of print]. [16] LiuC,HaoD,LiY,et al.Repair of facial scars using free and pedicle-expanded deltopectoral flaps[J].Br J Oral Maxillofac Surg,2021,59(6):710-715.DOI: 10.1016/j.bjoms.2020.12.022. [17] DingJ,LiY,LiW,et al.Use of expanded deltopectoral skin flaps for facial reconstruction after sizeable benign tumor resections[J].Am J Transl Res,2018,10(7):2158-2163. [18] MaX,LiY,LiW,et al.Reconstruction of large postburn facial-scalp scars by expanded pedicled deltopectoral flap and random scalp flap: technique improvements to enlarge the reconstructive territory[J].J Craniofac Surg,2017,28(6):1526-1530.DOI: 10.1097/SCS.0000000000003902. [19] KoshimaI,SoedaS.Inferior epigastric artery skin flaps without rectus abdominis muscle[J].Br J Plast Surg,1989,42(6):645-648.DOI: 10.1016/0007-1226(89)90075-1. [20] YuP,RoblinP,ChevrayP.Internal mammary artery perforator (IMAP) flap for tracheostoma reconstruction[J].Head Neck,2006,28(8):723-729.DOI: 10.1002/hed.20386. [21] VeselyMJ,MurrayDJ,NovakCB,et al.The internal mammary artery perforator flap: an anatomical study and a case report[J].Ann Plast Surg,2007,58(2):156-161.DOI: 10.1097/01.sap.0000232859.33035.d5. [22] SchellekensPP,HageJJ,PaesEC,et al.The internal mammary artery perforator pedicled island flap for reconstruction of the lower head and neck and supraclavicular region: how we do it[J].Clin Otolaryngol,2010,35(4):332-336.DOI: 10.1111/j.1749-4486.2010.02171.x. [23] SongB,ZhaoJ,GuoS,et al.Repair of facial scars by the free expanded deltopectoral flap[J].Plast Reconstr Surg,2013,131(2):200e-208e.DOI: 10.1097/PRS.0b013e3182789c02. [24] Saint-CyrM,SchaverienM,RohrichRJ.Preexpanded second intercostal space internal mammary artery pedicle perforator flap: case report and anatomical study[J].Plast Reconstr Surg,2009,123(6):1659-1664.DOI: 10.1097/PRS.0b013e3181a64eb0. [25] ZanT,LiH,DuZ,et al.Reconstruction of the face and neck with different types of pre-expanded anterior chest flaps: a comprehensive strategy for multiple techniques[J].J Plast Reconstr Aesthet Surg,2013,66(8):1074-1081.DOI: 10.1016/j.bjps.2013.04.028. [26] 昝涛,李海洲,顾斌,等.应用预构技术重建毁损脸面的12年经验总结[J].中华整形外科杂志,2018,34(7):503-509.DOI: 10.3760/cma.j.issn.1009-4598.2018.07.003. [27] ZanT,GaoY,LiH,et al.Pre-expanded, prefabricated monoblock perforator flap for total facial resurfacing[J].Clin Plast Surg,2017,44(1):163-170.DOI: 10.1016/j.cps.2016.08.007. [28] PalmerJH,TaylorGI.The vascular territories of the anterior chest wall[J].Br J Plast Surg,1986,39(3):287-299.DOI: 10.1016/0007-1226(86)90037-8. [29] 范冷艳,吴晋宝. 胸廓内血管及其穿支的应用解剖[J]. 解剖学杂志,1983,2(3):221-224. [30] GillisJA,PrasadV,MorrisSF.Three-dimensional analysis of the internal mammary artery perforator flap[J].Plast Reconstr Surg,2011,128(5):419e-426e.DOI: 10.1097/PRS.0b013e31822b7541. [31] 顾舒晨,李海洲,高雅姗,等.吲哚菁绿荧光造影在背部扩张穿支皮瓣设计中的应用[J].中华整形外科杂志,2020,36(3):251-256.DOI: 10.3760/cma.j.cn114453-20200218-00056. [32] 刘代明,黄昕,昝涛,等. 扩展穿支皮瓣血供范围的基础和临床研究进展[J]. 组织工程与重建外科杂志,2018, 14(2):101-104. DOI: 10.3969/j.issn.1673-0364.2018.02.011. [33] ZanT,LiH,HuangX,et al.Augmentation of perforator flap blood supply with sole or combined vascular supercharge and flap prefabrication for difficult head and neck reconstruction[J].Facial Plast Surg Aesthet Med,2020,22(6):441-448.DOI: 10.1089/fpsam.2020.0040. [34] HuangX,LiuD,GuS,et al.Augmentation of perforator flap blood supply with vascular supercharge or flap prefabrication: evaluation in a rat model[J].Plast Reconstr Surg,2021,147(5):1105-1115.DOI: 10.1097/PRS.0000000000007893. -
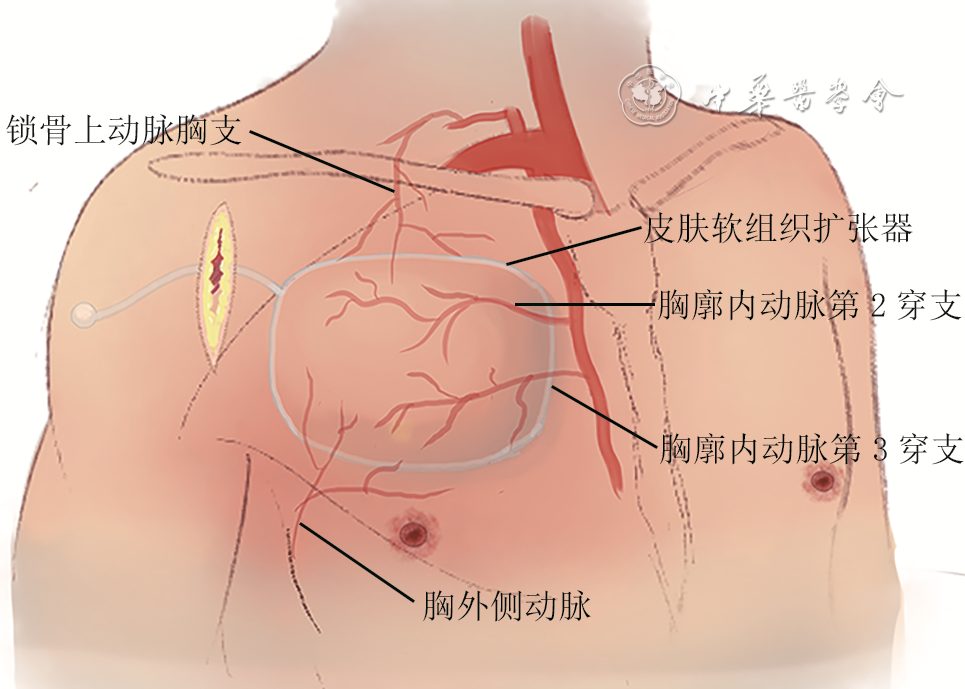
4 扩张的胸廓内动脉穿支(IMAP)+胸外侧动脉游离皮瓣整复例3患者面颈部烧伤后瘢痕。4A.Ⅱ期术前右侧颈部、胸部皮肤扩张及左面部瘢痕情况;4B.Ⅱ期术中游离皮瓣,解剖右侧胸廓内动脉第3穿支(黄色箭头)和胸外侧动脉(白色箭头);4C.Ⅱ期术中吲哚菁绿血管造影(ICGA)前皮瓣外观;4D.Ⅱ期术中夹闭胸外侧动脉,行ICGA显示IMAP最大灌注期供血不佳;4E.Ⅱ期术中夹闭IMAP,行ICGA显示胸外侧动脉最大灌注期供血不佳;4F.Ⅱ期术中同时开放IMAP和胸外侧动脉,再次行ICGA显示皮瓣血运良好;4G.Ⅱ期术中将右侧前胸皮瓣转移至左侧面颈部;4H.随访3年,中下面部皮瓣颜色、质地与周围正常皮肤相近,恢复了正常的下颌轮廓
-







 下载:
下载: